
Extensively drug-resistant tuberculosis
Tuberculosis that is resistant to the most effective drugs / From Wikipedia, the free encyclopedia
Dear Wikiwand AI, let's keep it short by simply answering these key questions:
Can you list the top facts and stats about XDR-TB?
Summarize this article for a 10 year old
Extensively drug-resistant tuberculosis (XDR-TB) is a form of tuberculosis caused by bacteria that are resistant to some of the most effective anti-TB drugs. XDR-TB strains have arisen after the mismanagement of individuals with multidrug-resistant TB (MDR-TB).
| Extensively drug-resistant tuberculosis | |
|---|---|
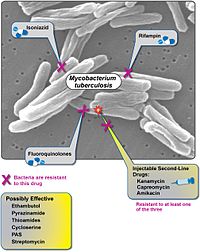 | |
| Description of extensively drug-resistant tuberculosis | |
| Specialty | Infectious diseases |
| Symptoms | The same as tuberculosis |
| Causes | Mycobacterium tuberculosis |
| Risk factors | Improperly treated tuberculosis |
Almost one in four people in the world is infected with TB bacteria.[1] Only when the bacteria become active do people become ill with TB. Bacteria become active as a result of anything that can reduce the person's immunity, such as HIV, advancing age, or some medical conditions. TB can usually be treated with a course of four standard, or first-line, anti-TB drugs (i.e., isoniazid, rifampin and any fluoroquinolone). If these drugs are misused or mismanaged, multidrug-resistant TB (MDR-TB) can develop. MDR-TB takes longer to treat with second-line drugs (i.e., amikacin, kanamycin, or capreomycin), which are more expensive and have more side-effects. XDR-TB can develop when these second-line drugs are also misused or mismanaged and become ineffective. The World Health Organization (WHO) defines XDR-TB as MDR-TB that is resistant to at least one fluoroquinolone and a second-line injectable drug (amikacin, capreomycin, or kanamycin).[2]
XDR-TB raises concerns of a future TB epidemic with restricted treatment options, and jeopardizes the major gains made in TB control and progress on reducing TB deaths among people living with HIV/AIDS. It is therefore vital that TB control be managed properly and new tools developed to prevent, treat and diagnose the disease.
The true scale of XDR-TB is unknown as many countries lack the necessary equipment and capacity to accurately diagnose it. By June 2008, 49 countries had confirmed cases of XDR-TB.[3] By the end of 2017, 127 WHO Member States reported a total of 10,800 cases of XDR-TB, and 8.5% of cases of MDR-TB in 2017 were estimated to have been XDR-TB.[2]
In August 2019, the Food and Drug Administration (FDA) approved the use of pretomanid in combination with bedaquiline and linezolid for treating a limited and specific population of adult patients with extensively drug resistant, treatment-intolerant or nonresponsive multidrug resistant pulmonary TB.[4]